Understanding the Root Causes of Comedonal Acne: The Science Behind Closed Comedones
- Introduction to Closed Comedones
- Causes of Closed Comedones
- Genetics and Hormones as Root Cause of Closed Comedones
- Factors That Contribute to Acne
- Prevention Techniques for Reducing the Appearance of Closed Comedones
- Use ‘Non-Comedogenic’ Skincare Products
- Follow Skincare Tips
- Maintain Proper Diet & Exercise
- Conclusion
- FAQs
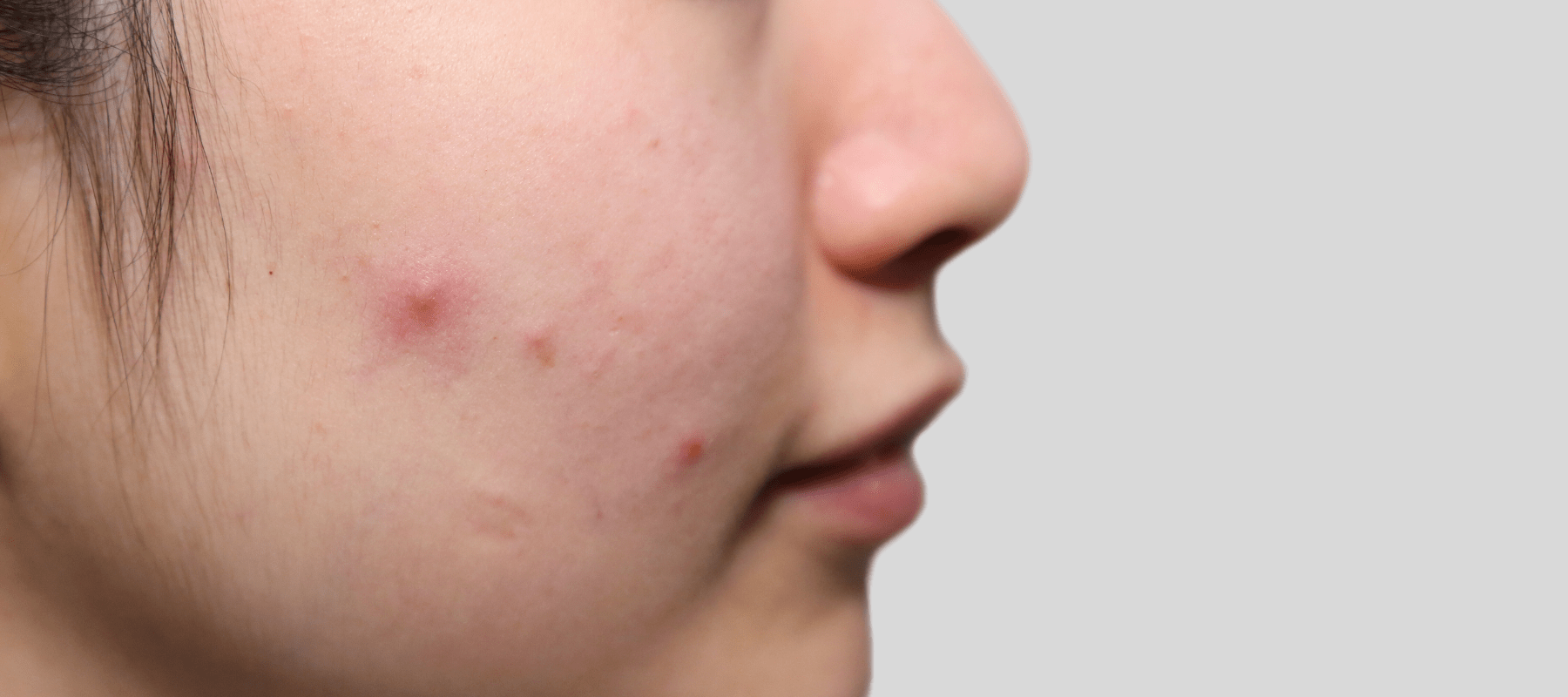
Introduction to Closed Comedones
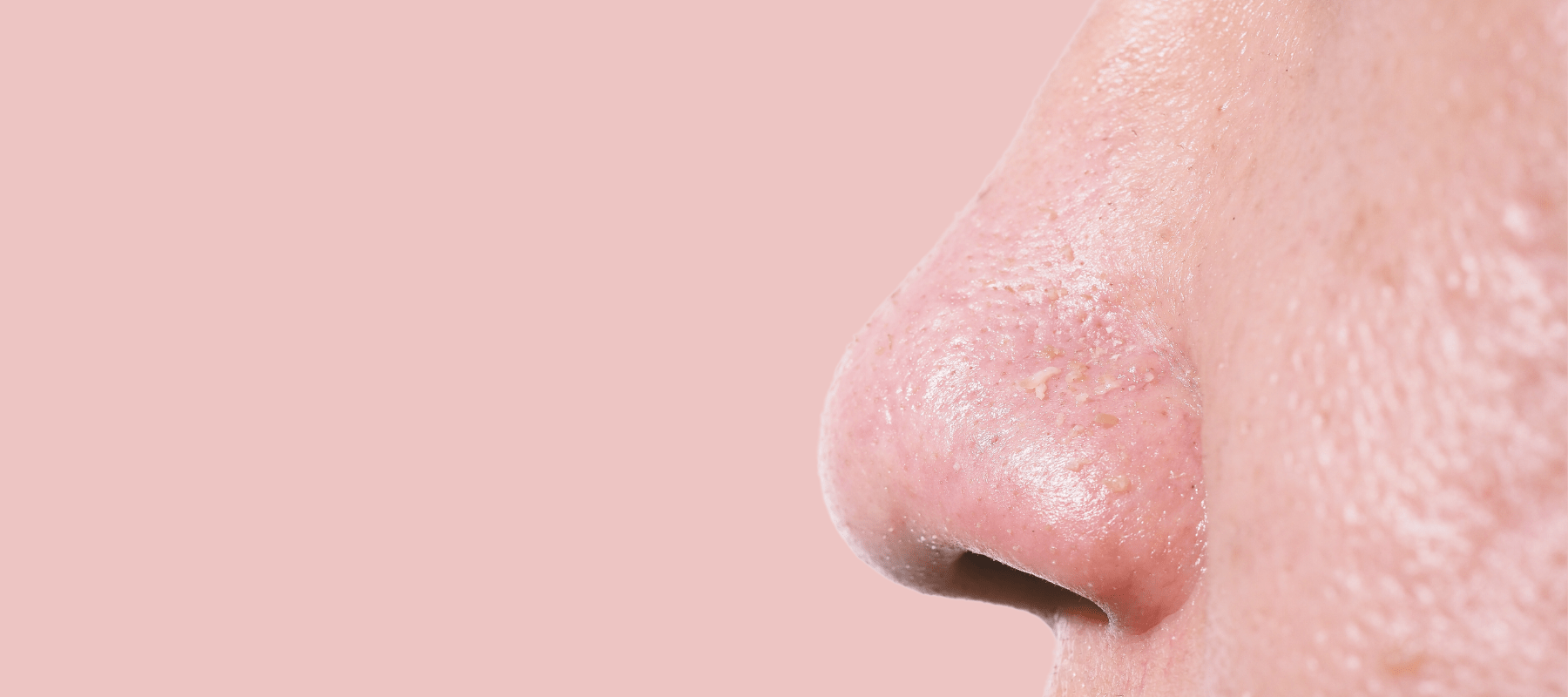
Closed comedones can be just as annoying despite not having the same flash as their red, inflamed siblings. These tiny, flesh-colored lumps make your skin look drab and uneven.
Although closed comedones are harmless, they occasionally cause more severe acne issues. This article discusses the primary causes of closed comedones. Also, you’ll learn how to deal with or avoid them here.
Causes of Closed Comedones
Comedones develop when sebum production increases and the sebaceous duct lining cells multiply. The material obstructs the hair follicle and sebaceous duct, causing a comedo. So, there’s no doubt that inflammation has a role in forming closed comedones.
Here is a list of elements contributing to comedonal acne causes:
- Excessive 5-testosterone (DHT) activity in skin cells.
- Reduction in linoleate in sebum, resulting in low barrier function.
- Acne-causing bacteria produce free fatty acids from sebum.
- Premenstrually moistened skin from moisturizers or in humid environments contact with some chemicals.
- Follicular rupture due to trauma such as pimple extraction, harsh cleaning, chemical peels, or laser treatments.
- Smokers experience comedonal acne more frequently than non-smokers.
- Certain dietary elements, especially dairy products and foods with a high glycaemic index.
Also read: 6 Effective Comedones Treatment Methods
Genetics and Hormones as Root Cause of Closed Comedones
Although various factors can result in closed comedones, heredity and hormones are two of the most typical underlying closed comedones causes.
Genetics
Closed comedones just occur more frequently in certain people than others. Genetics can affect how much oil your skin generates and how rapidly skin cells shed. Also, you’re more prone to get closed comedones if your family has a history of having them.
Hormones
Hormonal changes can also bring on closed comedones. This explains why stress, pregnancy, and puberty generally occur when closed comedones are more prevalent.
Your skin may generate more oil and exfoliate slower if your hormones are out of whack. So this may result in an accumulation of oil and dead skin cells within your hair follicles. Finally, this may form closed comedones.
Also read: Closed Comedones Treatment: Effective Ways for Clearing Your Skin
Factors That Contribute to Acne
A wide range of factors contribute to the development of acne, including:
Diet
Some research points to the possibility that certain meals may cause acne outbreaks. For instance, diets high in carbs or sugar can raise insulin levels, resulting in inflammation. The main cause of acne is inflammation.
Dairy products, processed meals, and foods high in saturated fat are more foods connected to acne. These meals can potentially contribute to excessive sebum production, a significant cause of acne.
Stress
Your body releases hormones under stress, including cortisol. Sebum, the oily material your skin creates to maintain moisture, can be produced more readily when cortisol is present. Excessive sebum can clog your pores, which can cause acne.
Skincare Products
Comedogenic chemicals are one of the most frequent ways skin care products can result in acne. Ingredients that are comedogenic might clog pores and cause outbreaks. Ingredients that are frequently comedogenic include:
- Lanolin
- Vegetable oil
- Beeswax
- Shea butter
- Mineral oil, etc.
It's crucial to stay away from products with these components if you suffer from acne-prone skin. Search for items with the designations "non-comedogenic" or "won't clog pores” like The Pink Foundry’s Acne Care & Healing Gel Moisturiser
Prevention Techniques for Reducing the Appearance of Closed Comedones
Trying to avoid comedonal acne completely is the best course of action. Lifestyle choices might complement any therapies that your healthcare professional suggests.
Use ‘Non-Comedogenic’ Skincare Products
Gel cleansers remove oil and debris from acne-prone skin. A water-based moisturizer is the best. Look for lotions designed for combination with oily skin if you have closed comedones on your face.
Purchase only non-comedogenic cosmetics to prevent pore clogging. Also, use sunscreen-containing foundation, particularly if you're using retinoids or acid-based peels.
Follow Skincare Tips
Ensure cleansing and moisturizing your skin twice every day. You should incorporate the following additional advice into your everyday routine:
- Spend at least 30 seconds gently massaging your face in circular strokes.
- No scraping at all!
- Apply witch hazel or an over-the-counter toner after.
- Before using sunscreen and makeup, let your moisturizer dry.
- After working out during the day, wash your face.
- Never go to bed wearing makeup because this can cause your pores to retain extra oil.
- Try a pre-cleanser to get rid of grease, makeup, and sunscreen.
Maintain Proper Diet & Exercise
Taking internal measures to manage comedonal acne is also beneficial. Diet and exercise may aid you in this situation. You should limit your dairy products, added sugars, and fat intake. According to some sources, these chemicals worsen comedones' underlying inflammation cause.
How to do it fast? Refrain from eating any sugary and processed food items. You could try a plant-based diet. These include lots of antioxidants, which can reduce inflammation and free radicals. These outcomes are also possible with regular exercise.
Conclusion
Comedones can occur at any age but are more frequent in adolescence. A significant component may be variations in hormone levels. Humidity and oily skin care products can also make it worse.
While you cannot control the hormonal factor, you can always use the best skin care products, like the ones from The Pink Foundry. Get the best serum and healing moisturizer from the house of TPF and bid goodbye to comedonal acne in no time!
FAQs
-
Can I get acne from closed comedones?
Closed comedones initially appear to be minor skin care annoyances, but if left untreated, they can develop into irate, inflamed pimples.
-
What pops out of comedonal acne?
The two types of comedones are whiteheads and blackheads. The majority of people have experienced comedonal acne.
-
Can Comedonal acne be permanent?
It's crucial to remember that comedonal acne needs ongoing care and therapy. There is always a chance of developing new comedones due to overactive sebaceous glands.

























































Leave a comment
This site is protected by hCaptcha and the hCaptcha Privacy Policy and Terms of Service apply.